MILWAUKEE — Over the past two years, the scientific world has seen a steady flow of research updating what we know about the novel coronavirus, SARS-CoV-2, and how it affects humans.
Because the virus is so new, researchers are still grappling with many questions about its function. And because of the nature of the scientific process, no single study can completely answer those questions. Instead, new research is constantly challenging our understanding of the pandemic.
Here, we explore some recent studies that have shed new light on the virus.
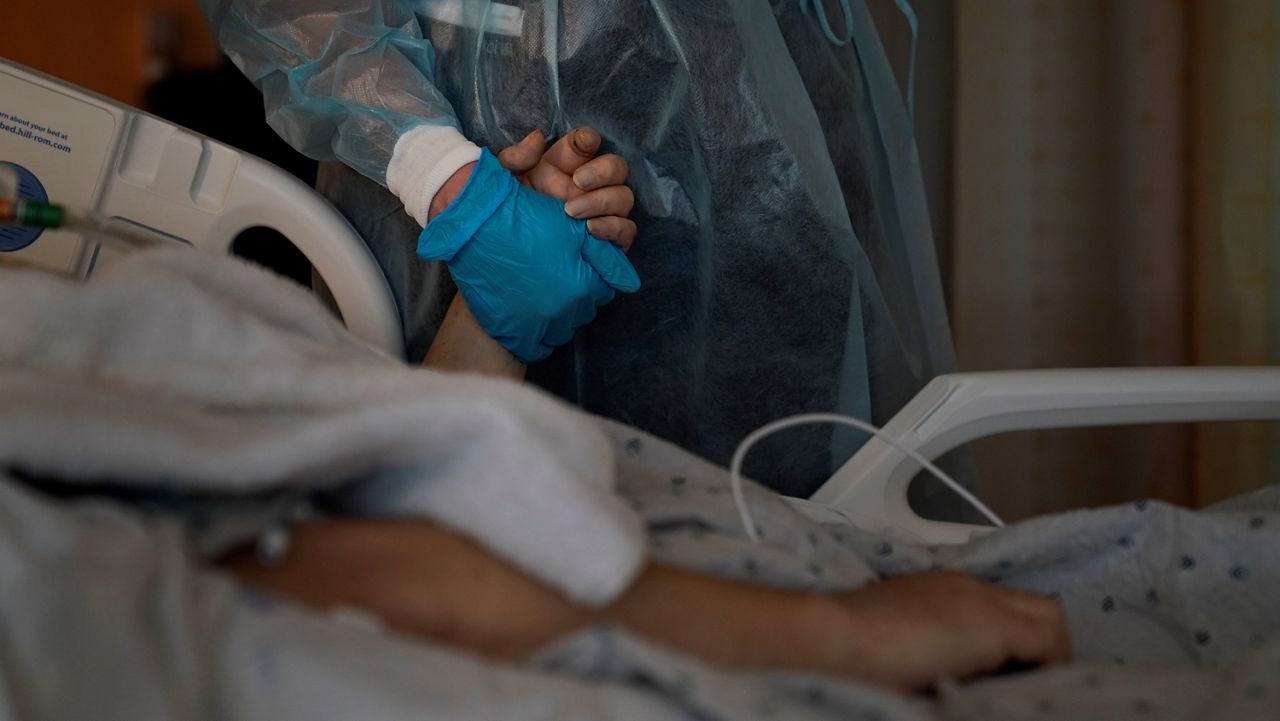
For health care workers and families, COVID-19 trauma is real
When a patient suffers from severe COVID-19, their caregivers’ mental health can suffer too, recent research has emphasized.
According to a study from Duke researchers, health care workers during COVID-19 had levels of “potential moral injury” (PMI) — a kind of post-traumatic stress — that were similar to the levels among military combat veterans.
Moral injury describes the damage done to someone’s conscience or identity when they see or do things that go against their own moral code, lead author Jason Nieuwsma explained in a press release.
The study compared potential moral injury in two groups of people: 618 military veterans who were deployed to a combat zone after 9/11, and 2,099 health care workers in the U.S. during the COVID-19 pandemic.
Out of these groups, 46% of veterans and 51% of health care workers reported experiencing “other-induced PMI,” or being disturbed by other people’s immoral acts. In addition, 24% of veterans and 18% of health care workers reported “self-induced PMI” — where they were disturbed by acting against their own moral code.
As the COVID-19 pandemic surged, health care workers reported many challenges that led to moral conflicts — like rationing care as hospitals grew overwhelmed, watching the public disregard public health guidelines and barring visitors from seeing dying patients.
"A lot of these people entered this profession because they want to provide care for people, they want to help other people," Nieuwsma told NBC. "I think for many folks that that's what has been challenged or ruptured."
And these moral conflicts were linked with negative outcomes: Health care workers with higher PMI levels reported lower quality of life and more depression and burnout, the study found.
Pandemic hospitalizations weren’t just taxing for the health care workers, either. Families of COVID-19 patients also experienced high levels of trauma, according to another study this week.
Researchers surveyed 330 people who’d seen family members admitted to intensive care for COVID-19. Most of the group — around 64% — reported significant symptoms of PTSD three months after the ICU stay, the study found.
That prevalence of PTSD symptoms was around twice as high as for ICU stays before the pandemic. Researchers suggested that visitation restrictions took an extra toll on family members — especially those who didn’t trust the clinicians to report back accurately on their loved ones.
“As the COVID-19 pandemic continues to challenge the ability of family members to build bedside relationships with clinicians, this loss of trust may translate to an increase in stress-related disorders,” the authors wrote.
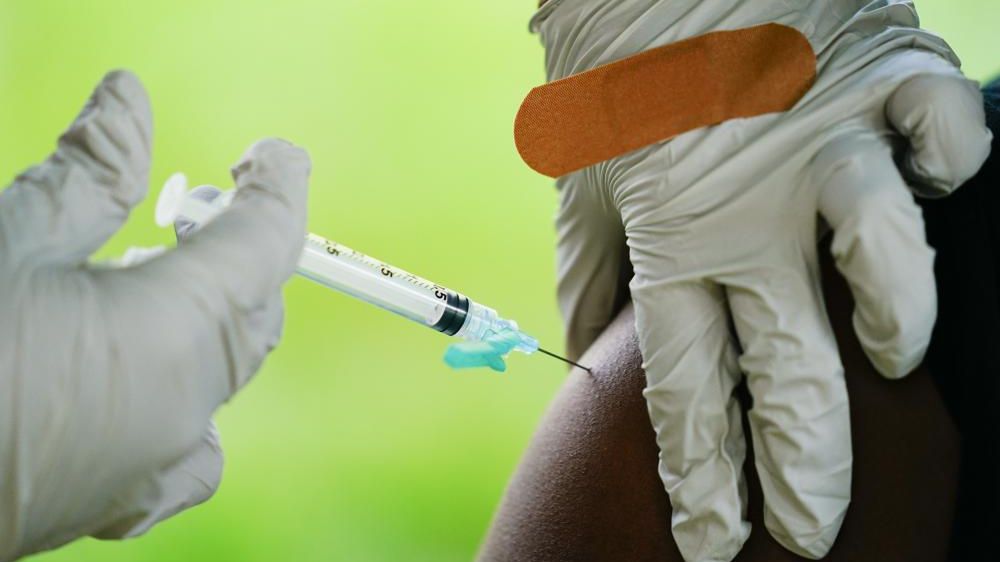
Bivalent vaccines show promise against coronavirus variants
Though our current vaccines still pack a punch against the virus’s worst effects, some vaccine makers are working on versions that can better protect against slippery new variants.
Pfizer and Moderna have been testing out a “bivalent” approach — shots that mix the original vaccine formula with a version that targets a particular variant.
And this month, Moderna announced promising results for one of these shots, which included genetic material from the beta variant.
The bivalent booster dose “demonstrated superiority against beta, delta and omicron variants of concern one month after administration,” Moderna reported.
Those preliminary results found that the bivalent shot produced twice-as-high levels of antibodies that could neutralize the omicron variant — even though omicron wasn’t specifically targeted in the vaccine.
More research is needed to confirm whether the bivalent shots will be the best path moving forward, STAT News reports. For example, Moderna’s research didn’t directly test whether these higher antibody levels would lead to better protection from infection or severe disease.
But the company said the bivalent approach is their main focus now, to keep antibody levels high while also helping the body respond to new variants.
“We believe that a bivalent booster vaccine, if authorized, would create a new tool as we continue to respond to emerging variants,” Stéphane Bancel, Chief Executive Officer of Moderna, said in a press release.
Moderna and Pfizer are both testing bivalent vaccines that target the omicron variant, to be used as possible boosters in the fall, NPR reports.
More evidence for the connection between COVID-19 and diabetes
The concerning link between catching COVID-19 and developing diabetes keeps getting stronger.
A large-scale study published in March found that people who recovered from COVID-19 had a greater risk of a new diabetes diagnosis, even if their initial infection was mild.
Researchers looked at health records from millions of patients — including around 180,000 who had recovered from COVID-19 — in Veterans Affairs databases. Compared to the control groups, the COVID-19 patients were around 40% more likely to develop diabetes within a year of their infection, the researchers found.
The diabetes rates were higher for those who had more severe COVID-19 infections, according to the study. But even those who weren’t hospitalized still saw a jump in their diabetes risk.
Almost all of these new diagnoses were type 2 diabetes, rather than type 1, the research found. And certain groups had a higher risk of developing diabetes after COVID-19, including Black patients and older adults over 65.
Overall, around 1 to 2% of those who recover from COVID-19 may develop diabetes, the study estimates. It’s a small portion, but can add up to a significant burden given the high number of people who have gotten COVID-19.
“When this whole pandemic recedes, we’re going to be left with the legacy of this pandemic — a legacy of chronic disease,” study co-author Ziyad Al-Aly told Nature.
More research is needed to figure out where this link might be coming from, but there are a few possible pathways, as The Conversation reports — like inflammation from a COVID-19 infection making the body resistant to insulin, or the coronavirus infecting cells that produce insulin.
And the risk runs both ways: Studies have also continued to show that people with diabetes are more likely to face severe outcomes from COVID-19. Diabetes patients may account for upwards of 30% of COVID-19 deaths, according to data from the CDC.
“Diabetes is a wicked problem and COVID has just shone a bright light on this crisis,” Dr. David Kerr of the Sansum Diabetes Research Institute told The New York Times.
Keeping tabs on variants as they splinter off and swap genetic code
These days, scientists are tracking a wide range of variants and subvariants as the virus continues to split off and recombine into new forms.
The coronavirus that continues to spread today looks a lot different from the one that kicked off the pandemic more than two years ago. And even omicron — the latest variant of concern to get a full Greek letter name — has kept transforming since it first sparked the winter surge, quickly evolving into new forms, as the World Health Organization said in a recent report.
The coronavirus variant that first got the name “omicron” back in December was technically a lineage known as B.1.1.529.
But since then, we’ve seen omicron splinter off into different versions, with BA.1 and BA.2 — subvariants that still share many of the same mutations as the original omicron — taking over in the U.S. one after the other. Scientists have already identified several other “sister” subvariants, too, all the way through BA.5.
Now, a subvariant known as BA.2.12.1 — which is a sublineage that’s kind of like a daughter to BA.2 — is on the rise in the U.S., making up almost 30% of new cases in the CDC’s latest estimates.
Sequencing has also detected “recombinant” versions of the virus — ones where different variants have mixed and matched some of their genetic material.
These combo variants can happen when two versions of the virus infect a cell at the same time, as New Scientist explains. As the virus makes copies of itself in the cell, one variant may end up picking up pieces of the other variant’s genome.
Recombinant versions of the coronavirus have probably been happening since early in the pandemic, as The Atlantic explains. But because today’s variants look so different from each other, it’s easier to tell when they swap some genetic material.
Scientists have already found a couple of “deltacron” variants that bring together pieces of the omicron and delta variants, including ones with the technical names XD and XF.
And several recombinant variants include multiple versions of omicron — including XE, which brings together both BA.1 and BA.2.
So far, though, these mix-and-match variants haven’t spread very widely, and experts say that our immunity from other versions of the virus should hold up against recombinant variants.
Other news to note:
Most Americans have already been infected by the coronavirus, according to recent CDC estimates. After testing more than 200,000 people for antibodies, the CDC found that almost 60% showed signs of prior infection — including around three-quarters of all kids in the U.S.
Though sexually transmitted diseases dropped in the U.S. during the early months of the pandemic, by the end of 2020 they had surged past 2019 totals, per a CDC study this month. Overall, 2020 saw cases of gonorrhea and syphilis jump by around 10%, researchers found, pointing to disruptions in health care as a possible factor in the increase.
The FDA authorized the first COVID-19 treatment for kids under 12 when it gave the green light to use remdesivir in younger children. The antiviral medicine is now available to treat COVID-19 cases in kids as young as 28 days old, the FDA announced at the end of April.
During the omicron wave, kids aged 5 to 11 were more than twice as likely to be hospitalized from COVID-19 than their vaccinated peers, the CDC found in a recent analysis. Almost 90% of hospitalized children in this age group were unvaccinated, the study found, even though they were eligible for their shots during the study period.