CLEVELAND — The Ohio Coronavirus Wastewater Monitoring Network is made up of the Ohio Department of Health, the Ohio Environmental Protection Agency, the U.S. Environmental Protection Agency, and the Ohio Water Resources Center at the Ohio State University, the University of Toledo, Kent State University and the University of Akron.
Together, they look for early warning signs of the virus in order to help communities get ahead of the spread of the disease and make informed decisions about how to respond, such as setting up vaccination clinics or test sites.
COVID-19 variants can be found in wastewater samples up to a week before an outbreak develops.
They can also tell the difference between variants showing up in human waste.
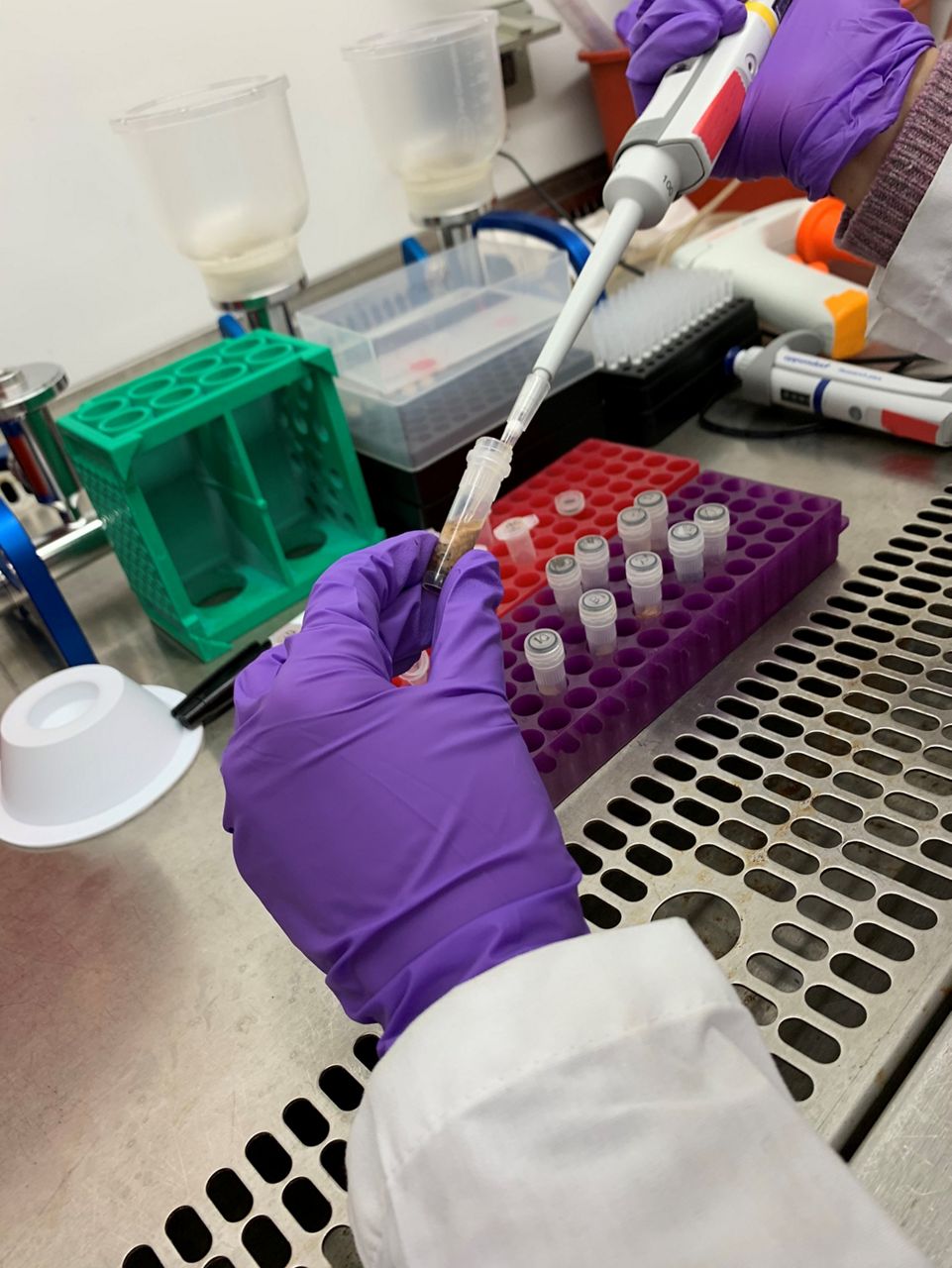
“It’s spreading,” explained Zuzana Bohrerova, research specialist in the Department of Civil, Environmental and Geodetic Engineering, and associate director of the Ohio Water Resources Center at Ohio State University. “It’s not overtaking delta; we now have a mixture of both delta and omicron in the state.”
Wastewater plants throughout Ohio have been submitting samples to the network for its research since the start of the pandemic.
“Almost everything you can see in wastewater, including biological or chemical markers,” said Bohrerova.
The Ohio Department of Health has a map that shows all wastewater centers in the state, and the ones with the red dots are where COVID-19 samples are substantially increasing.
The information gives communities a head start to prepare for outbreaks.
The Ohio Department of Health gives these examples of how the wastewater testing can help the state:
- Serve as an early warning of infection in communities or congregate settings.
- Provide information that can help local communities more quickly intervene with protective measures to slow disease spread.
- Help communities measure the effectiveness of such interventions (quarantine/face coverings/business limitations).
- Develop methodologies/predictive models to translate viral loads detected for comparison with other data, such as rates or percentage of infection in communities.
- Where possible, compare results to previously collected data on prevalence in specific communities to better understand factors affecting disease spread.
- Determine impacts on disproportionately affected communities or communities where risk of infection is greater.
Click this link for more information on this collaborative effort.










