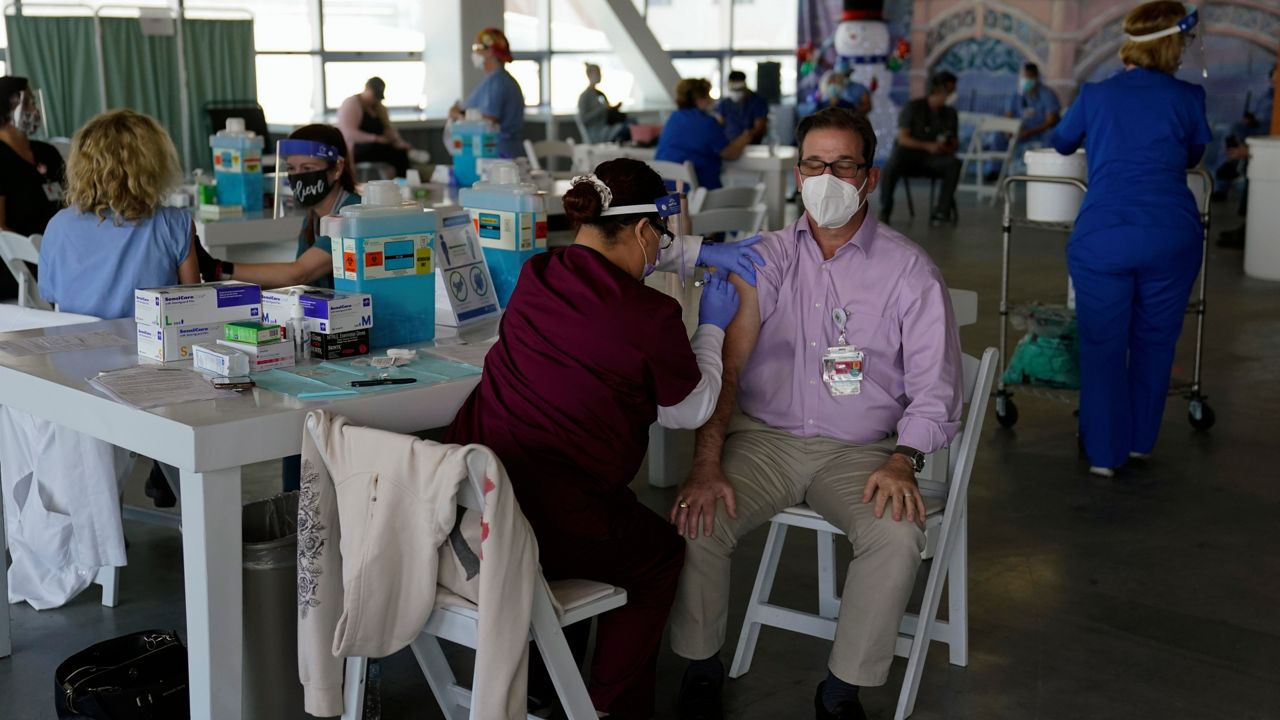
SANTA ANA, Calif. (CNS) — Orange County's weekly averages for COVID-19 cases and positivity rates ticked up after several weeks of gradual decline, according to data released Tuesday by the Orange County Health Care Agency.
The county's weekly COVID-19 case rate per 100,000 residents, which is released on Tuesdays, increased from 6 to 7.2, while the test-positivity rate ticked up from 2.3% to 2.5%. The county's Health Equity Quartile positivity rate — which measures progress in low-income communities — inched up from 2.3% to 2.4%.
Hospitalizations due to the coronavirus decreased from 199 on Monday to 197, with the number of intensive care unit patients decreasing from 53 to 47.
The county has 23.1% of its intensive care unit beds available and 69% of its ventilators.
The county also reported 169 more infections Tuesday, raising the cumulative total from throughout the pandemic to 305,788. Two more fatalities logged Tuesday increased the death toll to 5,602.
The hospitalization numbers being reported reflect patients who are primarily being treated for COVID-19, according to Deputy County Health Officer Dr. Regina Chinsio-Kwong.
Previously, many of those listed as COVID-19 patients just happened to have the virus but were in the hospital for some other reason and subjected to mandatory testing.
The case rate among the unvaccinated has seen a marked increase, and a slight increase among the vaccinated has also been detected, according to the OCHCA.
The case rate per 100,000 unvaccinated residents was 14 on Oct. 16, but increased to 15.7 as of Oct. 23, the latest data available. For fully vaccinated residents it was 2.8 on Oct. 16, but 3.4 per 100,000 residents by Oct. 23.
Dr. Dan Cooper, a pediatrician with UC Irvine's Institute for Immunology, said he is advising parents to get their 5- to 11-year-old children vaccinated now that the Centers for Disease Control has approved the Pfizer vaccine in that age group.
However, he is careful to tell reluctant parents to at least think about it. He does not favor mandates.
"I would at first like to try to get parents to get the vaccine," Cooper told new sources. "It's a touchy situation. You're making a decision about someone else, not about yourself."
Cooper noted that "because it is less severe" a problem among children, "we have a little bit more breathing room."
So Cooper is "going to urge parents to get the vaccine," but, he added, "Should it be mandated? I don't know yet. Mandating could do more harm than good. In the end you may not vaccinate more kids."
Cooper said it appears one-third of the parents of his patients want to get their children vaccinated right away, one-third is reluctant but open minded down the line and another third is just against it.
Cooper said his practice mostly treats low-income Latino families and many parents "have been so affected by the disease they want their kids vaccinated as soon as possible."
But there is more hesitancy in communities not affected as much by COVID-19, Cooper said.
Cooper noted that while COVID-19 has not had as much effect on children that doesn't mean they're not at risk of the disease.
"I don't buy the data that it is completely innocuous in children because it is not," Cooper said. "There are going to be kids with no underlying conditions who are going to get very sick."
Also, the experts do not know what long-term effects COVID-19 could have on some children.
Cooper has done much research into the obesity epidemic among children and that overweight children are not only more susceptible to serious symptoms they also get less protection from the vaccines.
"It's as true in children as it is true in adults," Cooper said. "I'm hoping one of the lessons from this whole thing is we need to resume our efforts to deal with obesity and inactivity in kids. It's an epidemic."
The two deaths logged Tuesday occurred in October, raising last month's death toll to 49.
September's death toll stands at 167, close behind August's death toll of 172.
In contrast, the death toll before the more contagious delta variant-fueled surge was 29 in July, 19 for June, 26 for May, 46 for April, 200 for March, 615 for February, 1,585 for January — the deadliest month of the pandemic — and 977 for December, the next-deadliest.